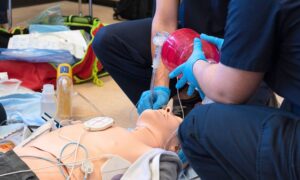
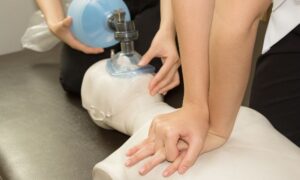
Study finds heart attacks are on the rise in young women between the ages of 35 and 54.
Shawn Sherlock was a healthy 44-year-old mom who ate right and ran regularly. She thought she was in great health until January 2017 when she had a heart attack one morning.
“I thought, this could not be a heart attack,” Sherlock remembers. “I am too young and healthy.”
But something told Sherlock she’d better take this seriously. “I thought, I don’t want my boys to see me drop dead in front of them,” the Boca Raton, Florida, businesswoman told NBC News.
Recent Trends
In recent years, there has been a trend of heart attacks in younger people, specifically younger women.
“The greater percentage of heart attacks among younger patients is alarming,” said study co-author Melissa Caughey, an instructor at the University of North Carolina School of Medicine in Chapel Hill. “And that’s especially true in light of the fact that the population is aging.”
The damage sustained in a heart attack can lead to heart failure and other issues later in life, Caughey explained.
Caughey and her colleagues explored heart attack trends using data from the Atherosclerosis Risk in Communities (ARIC) Study, which has been tracking hospitalizations for heart attacks in four geographically defined regions of the U.S. (Forsyth County, North Carolina; Washington County, Maryland; Jackson, Mississippi; and eight suburbs of Minneapolis, Minnesota).
Along with the dramatic increase in heart attacks in young women, the researchers also found that these hospitalized women were less likely than their male counterparts to receive guideline-recommended medications such as non-aspirin blood thinners (17 percent lower), cholesterol- lowering drugs (13 percent lower) and beta-blockers (4 percent lower). They were also 21 percent less likely than men to receive therapies to open clogged arteries.
“This is a very important study,” said Dr. Erin Michos, an associate professor of medicine and epidemiology and associate director of the Ciccarone Center for the Prevention of Cardiovascular Disease at Johns Hopkins University School of Medicine in Maryland. “The main message to women is you shouldn’t think you’re too young for a heart attack. There has always been a misconception that this is just a man’s disease…”
Younger Women May Not Be Getting Screened for Heart Disease Risk Factors
Another issue is that many women and doctors believe that there is less risk of a heart attack before menopause. And because of that, many younger women are not getting screened for heart disease risk factors, she said.
“In this study, more than 90 percent had modifiable risk factors, such as smoking, diabetes, high cholesterol and hypertension,” Michos said.
Part of the problem may lie in doctors’ perceptions of women, said Dr. Elizabeth Piccione, an assistant professor of medicine at the University of Pittsburgh Medical Center and a cardiologist with the UPMC Magee-Womens Heart Program.
For example, if a woman comes in and has high blood pressure she’s often told it’s because she’s anxious, Piccione said. When a man comes in with the same numbers, he’s told his blood pressure is high, she added.
“The number one thing that is going to kill and disable women is cardiovascular disease,” Piccione said. “One of the things we can take away from this study is that we are not aggressively treating women when we identify cardiovascular risk factors,” she added.
Preeclampsia Could Also Increase a Woman’s Risk of Heart Disease
One risk factor that many women and doctors don’t know about involves pregnancy, Michos said. Preeclampsia is a complication that strikes some women after 20 weeks of pregnancy. Its symptoms include high blood pressure and signs of damage to the liver and/or kidneys. Untreated, it can be fatal.
That study highlights the importance of keeping a close eye on women who had preeclampsia during pregnancy for signs that heart disease may be developing, Michos said.
Those results might help explain Sherlock’s heart attack at age 44. During her first pregnancy she developed preeclampsia, which progressed to full eclampsia, complete with seizures and the beginnings of organ failure.
Moving More Could Help Lower Risk
Another important, modifiable risk factor may be the amount of time women spend sitting, experts said. A study published in the same issue of Circulation found that older women who spent fewer hours sitting or who frequently got up and walked around before sitting back down had a significantly lower risk of heart disease.
That study followed 5,638 women aged 63 to 97 who had no history of heart attack or stroke. At the beginning of the study the women wore a device called an accelerometer for a week. The device kept track of when the women sat or reclined and when they got up.
At the end of the study, nearly five years later, the researchers determined that for each additional hour the women spent not sitting, there was a 12 percent lower risk of any type of cardiovascular disease and a 26 percent lower risk of heart disease.
Source: TODAY